Procedures
These are the most common procedures performed at CEAPS. We perform minimally invasive approaches for most of our procedures. Dr. Moawad believes that there is no condition too complex for a minimally invasive surgery, and has spent his career training, advocating and speaking about such techniques.
Endometriosis Excision is a procedure that removes Endometriotic lesions that could be located in the pelvis or outside the pelvis depending on your case. The removal of all endometriotic lesions is essential to relieving the pain caused by this disease.
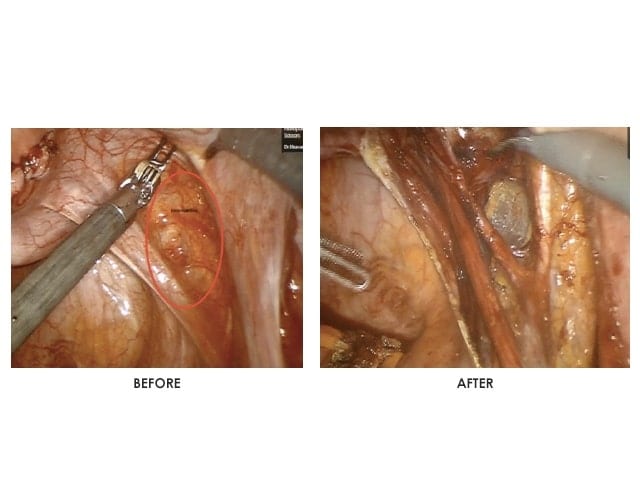
This procedure is minimally invasive through Laparoscopy or Robotic Surgery, and allows for management of pain and infertility associated with Endometriosis. It is the gold standard to manage this condition.
Endometriosis excision requires advanced surgical skills and well trained surgeons, especially in cases of deeply infiltrating endometriosis, where the surgical anatomy is challenging for inexperienced surgeons.
Endometriosis Excision, through only a few small skin incisions, using a thin camera that is inserted into the pelvic area, allows the endometriotic lesions to be cut out and removed.
Endometriosis treatment requires a comprehensive management plan set up with your doctor. Excision followed by appropriate management could help reduce the risk of recurrence of the disease.
While recovering from an Endometriosis Excision, you may experience:
- Pain that should resolve daily
- Pain around site of incisions
- Chest and shoulder pain
- Vaginal spotting
- Nausea caused by anesthesia or pain medication
- Swelling of arms and legs due to fluid retention
- Swelling of the abdomen due to irritation of intestines
- Constipation
- Diarrhea caused by antibiotics
- Urinary retention
- Bruises or scars around the incision areas
You should be able to get back to full activity and work shortly after the procedure. This depends on each patient and their personal recovery time.
Sex should be avoided for at least 2 weeks after the procedure, and should only resume once you are feeling comfortable.
Dr. Moawad is a fellowship-trained surgeon with a decade of experience in successful minimally invasive procedures. With both an international and national reputation, and working along with patient advocacy groups and educational platforms, Dr. Moawad continues to educate and publish his work on these kinds of procedures gaining expertise and credibility around the world.
At CEAPS, we believe in offering options that guarantee better outcomes for our patients. As Dr. Moawad puts it, “There is no condition too complex for minimally invasive surgery.” We exhaust all options before opting for open surgery as a last resort.
A Hysterectomy is a gynecological procedure that usually entails removing the entire uterus, including the cervix. There are different types of hysterectomies: Supracervical Hysterectomy, which entails removing the uterus while leaving the cervix in place, and Total Hysterectomy, which entails removing the uterus along with the cervix.
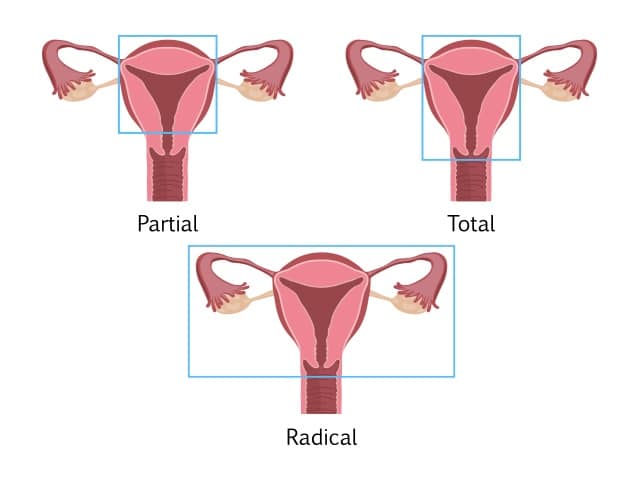
The term Hysterectomy, whether total or supracervical, is only specific to surgery on the uterus and does not include removal of the ovaries.
Removing the ovaries along with the uterus is not recommended in patients under 65 years old, unless indicated by your doctor. Removing the ovaries with a Hysterectomy is referred to as Oopherectomy.
It is recommended at the time of Hysterectomy to remove the fallopian tubes as well. Studies have shown that removing the fallopian tubes during a Hysterectomy can decrease the risk of future cancer of the ovaries and fallopian tubes by 30%.
Hysterectomies are performed to relieve the following conditions:
- Adenomyosis
- As part of pelvic prolapse repair
- Heavy bleeding, with or without Fibroids
- Pelvic pain with origin in the uterus
- Painful intercourse with origin in the uterus
At CEAPS, our preferred method of performing Hysterectomies is through a minimally invasive approach that could be done successfully in almost all cases, irrelevant of the size of the uterus or the complexity of the procedure.
This technique carries lower risks of complications and requires only small incisions, resulting in quicker recovery.
This procedure is ideal as it gives full access to the pelvis, allowing the doctor to evaluate and treat potential associated conditions, such endometriosis, scar tissue, and ovarian cysts.
After a Hysterectomy, people can be discharged the same day, and be back to their full, normal activity in around 2 weeks typically (aside from sex).
Sexual intercourse should only be resumed after at least 8 weeks, and only if you are feeling comfortable.
You might experience the following after a Hysterectomy:
- General pain that should resolve with time
- Pain around the incisions that should last only a few days
- Pelvic and rectal pain and pressure that should resolve with time
- Chest and shoulder pain that should resolve 2 to 3 days
- Bruises at the incisions that will resolve on their own
- Vaginal spotting during the first week
- Nausea caused by anesthesia and pain medication
- Swelling of the abdomen that will resolve over time
- Constipation due to medication
- Diarrhea caused by antibiotics
- Urinary retention due to anesthetics (seek your doctor’s advice if this occurs after you are sent home)
As part of your recovery, you might be given prescription medication to ease pain. It is important not to drive when taking any prescribed narcotics. Avoid lifting, swimming, and heavy exercise, and use caution when starting an exercise routine after your procedure, starting slowly and listening to your body to make sure you are comfortable and able.
A Hysterectomy will cause periods to stop, however hormone production should not be affected if ovaries are spared during the surgery. After a hysterectomy you are not able to conceive, so this procedure is not recommended for people desiring fertility or childbearing.
A Hysterectomy will not cause early menopause unless both of the ovaries have been removed during the procedure. In this case, Estrogen replacement therapy can be used to prevent menopausal symptoms, such as hot flashes, vaginal dryness, and night sweats. You can discuss this with your doctor, based on the procedure you undergo and what is best for your body.
Dr. Moawad has had a high success rate of minimally invasive surgeries over the past 10 years, and his work is all about exhausting every option before turning to open surgery as a last resort. With international and national distinction and published work in the field of minimally invasive surgery, along with his work with patients in advocacy groups, Dr. Moawad puts the patient’s wellbeing and recovery above all else.
At CEAPS, we work in the same spirit, performing successful minimally invasive procedures that make the patient’s life easier by shortening recovery time and improving outcomes.
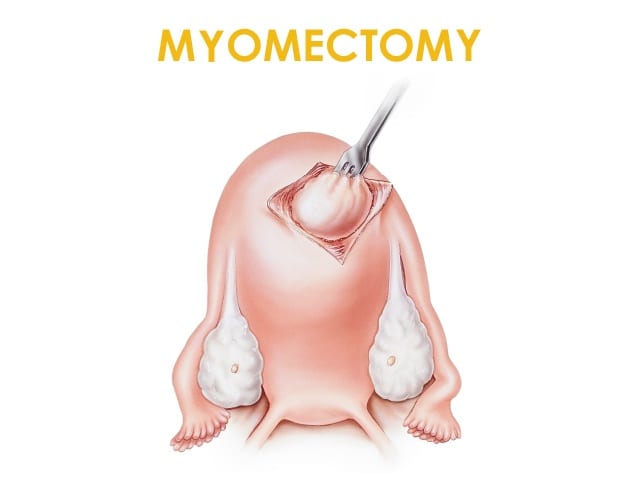
A Myomectomy is a surgical procedure to remove Fibroids, while keeping the uterus in place. Fibroids can lead to, abnormal uterine bleeding, difficulty conceiving, miscarriages, large and bulky uterus, and other serious complications during pregnancy.
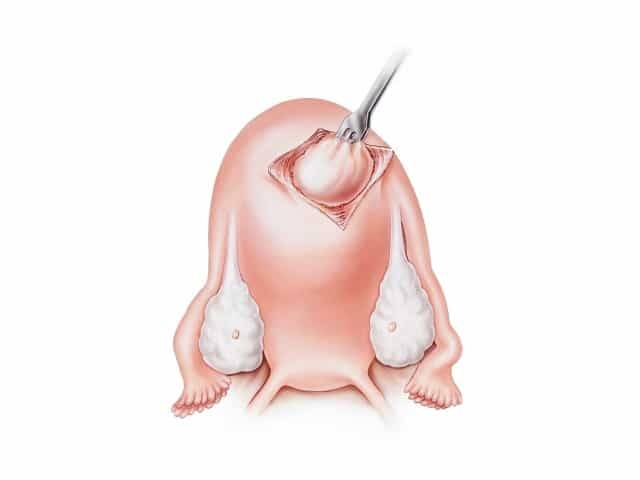
A Myomectomy is suggested for people with fibroids who still wish to maintain their fertility.
This procedure is rarely performed on people who no longer wish to have children.
Your doctor, following examinations, and depending on the location of the fibroids and their type, will determine the type of Myomectomy you need.
Depending on the location of fibroids and your symptoms, a hysteroscopic or a laparoscopic myomectomy could be offered by your surgeon.
Unfortunately many patients are still offered a traditional Myomectomy, mainly due to the complexity of their case (large or multiple fibroids) and the inexperience of their surgeon.
Minimally invasive and robotic surgeries are always an option for patients at CEAPS, even in the case of complex Myomectomies.
Recovering from a Myomectomy takes approximately 2 weeks, with patients getting back to work and normal activity within 7 to 10 days.
Sex should be avoided for at least two weeks after the procedure, and only resumed once you are feeling comfortable.
After your procedure, and depending on the technique used, you might experience the following:
- Bruises or scars at the incision sites
- Bleeding and spotting similar to menstruation a few days after surgery
- Swelling in arms and legs due to increase fluid intake during your procedure
- Swelling in abdominal area
- Constipation due do medication
- Diarrhea caused by antibiotics
- Urinary retention
- Pain around incision sites
- Pain in pelvic and rectal areas
- Chest and shoulder pain
- Nausea due to anesthesia and/or medication
It is important to be cautious about starting an exercise routine after surgery. Listen to your body and respects its limits.
After a Myomectomy, fertility will be retained, but it is important to allow the uterus to heal completely before trying to conceive. Be sure to consult your doctor about this.
Dr. Moawad believes in a minimally invasive approach for all procedures, performing almost all of his procedures over the past decade through this approach. With an extensive experience in myomectomy procedures, and national and international publications on the topic, Dr. Moawad is one of the world leading experts in performing these particular procedures. At CEAPS, with Dr. Moawad’s approach at the center of what we do, we are determined to provide the best minimally invasive surgeries, giving our patients quicker and easier recovery.
An Ovarian Cystectomy is the removal of ovarian cysts or tumors, while still preserving the ovaries.
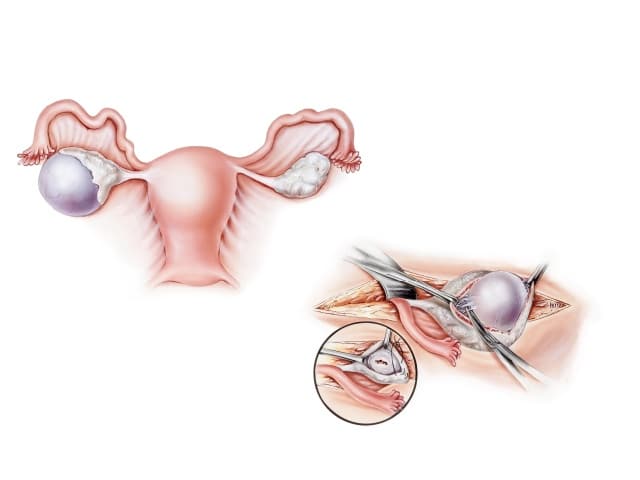
Ovarian cysts are common, and your doctor can decide on the best treatment and procedure for you based on the size and the type of the cyst or tumor, your age, and possible malignancy.
An Ovarian Cystectomy almost always is done with a minimally invasive procedure that involves small skin incisions, using laparoscopic or robotic techniques.
If a cyst is suspected to be malignant, full removal of the ovary might be necessary in order to avoid rupturing and spread of the cancerous cells into the pelvic area.
Removing of the cyst from the ovary can affect your ovarian reserve. Discuss with your doctor the best approach. Ovarian cystectomy requires an experienced surgeon that could minimize the damage to healthy ovarian tissues during the procedure and minimize the damage to the ovary.
Once the cyst is removed successfully, it is always sent for testing to rule out malignancy.
After a minimally invasive procedure, recovery is quick and pain is usually minimal. This procedure is an outpatient procedure, and patients are up walking within hours.
Patients can usually go back to normal activity and work within 1-2 weeks.
To relieve pain, your doctor may prescribe you medication.
Dr. Moawad applies a minimally invasive technique on all of his patients’ procedures, with a 10-year streak of high sucees in minimally invasive surgeries for various conditions. His international and national reputation, paired with his publications, successful procedures, and support for patient advocacy groups, has created an atmosphere of trust and accomplishment. At CEAPS, we work on empowering our patients with an optimal minimally invasive approach that will lead to a quick recovery and fast return to normal activity while improving their quality of life.
Cervical Insufficiency, also known as Cervical Incompetence, can be corrected through a procedure called a Cervical Cerclage.
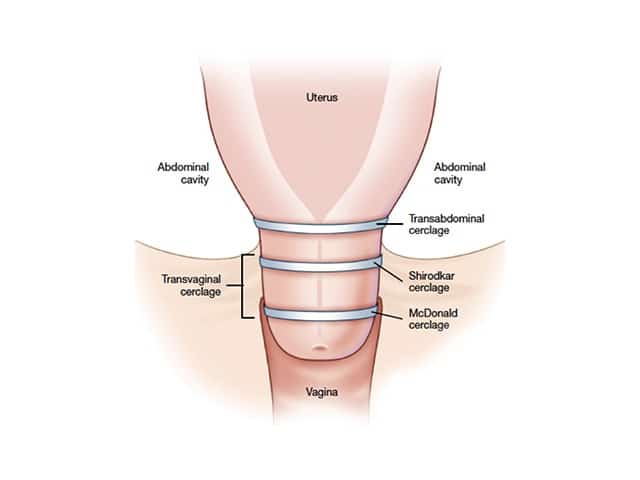
Transabdominal cerclage (TAC) is reserved for select people with previous failed transvaginal cerclage (TVC) and/or anatomic limitations to TVC placement due to short or absent cervix.
TAC is performed through laparoscopic/robotic approaches, with the extensive expertise and hands on experience of Dr. Gaby Moawad.
The indications for TAC include previous failed TVC and/or cervical anomaly, including history of congenital anomaly (short or absent cervix) or extensive cervical laceration or cervical surgery like LEEP in cases of precancerous lesions or cancer of the cervix.
The minimally invasive approach of a laparoscopic or robotic procedure offers a smoother and more stress-free experience with minimal recovery time and highly successful outcomes.
Transabdominal cerclage involves placing a tied loop high onto the cervix, helping reinforce the cervix and support it, preventing it from opening during pregnancy pre-term, while keeping the blood flow from the uterine artery unaffected.
After a Transabdominal cerclage, you should rest and avoid heavy activity and lifting heavy objects. Your doctor can guide you further on how to proceed after your procedure if you are pregnant.
With both an international and national reputation, Dr. Moawad is a fellowship-trained surgeon with a decade of experience in performing successful minimally invasive abdominal cerclages. Dr. Moawad continues to educate and publish his work on these kinds of minimally invasive procedures, gaining expertise and credibility around the world.
At CEAPS, we believe in offering options that guarantee better outcomes for our patients. As Dr. Moawad puts it, “There is no condition too complex for minimally invasive surgery.” We exhaust all options before opting for open surgery as a last resort.
An oophorectomy is a surgical procedure during which one or both of your ovaries are removed.
Why would you remove your ovaries?
There are several reasons for which you might need an oophorectomy. Below are the most common ones:
- A tubo-ovarian abscess, which is a pus-filled sac involving your fallopian tube and ovary. This is usually the result of an untreated infection. An abscess usually presents with fever and pelvic pain.
- Ovarian cancer: oophorectomy can be either therapeutic to remove the tumor or prophylactic to prevent the development of a cancer if you are known to have a genetic predisposition.
- Ovarian endometriosis or other benign cysts which might cause pelvic pain, period irregularities, ovarian torsion and infertility. Removal of the pathology can help relieve symptoms. For benign conditions like endometriosis and cysts removal of an ovary should be the last resort to treat these pathologies, an ovarian sparing approach should be always attempted.
- Ectopic pregnancy, which is pregnancy that implants in the tube or on the ovary. Ectopic pregnancies are not viable and if the sac and embryo get too big for medical treatment, you might need to have them removed surgically.
Oophorectomy can be unilateral if fertility is still desired or bilateral if fertility is no longer desired or if medically indicated. The removal of the ovary is sometimes accompanied by the removal of the fallopian tube as well depending on the extent of pathology and this procedure is termed salpingo-oophorectomy.
Your gynecologist will offer you the type of surgery that best treats your condition while keeping in mind your desire for future fertility.
Oophorectomy, like other surgeries, can be done via laparoscopy or using the robot and remain minimally invasive as opposed to an open approach that leaves the patient with a big scar and higher rates of complications.
A minimally invasive approach will allow you to leave the hospital within a day from the operation. Laparoscopy and robot-assisted surgery also speeds up the recovery process and gets you back to normal activity within 2 weeks.
At CEAPS, we always opt for minimally invasive approaches to provide the best experience for our patients with the least amount of side effects and complications. Ovarian sparing surgery is always the first line therapy for benign ovarian pathology.
Dr. Moawad is a highly reputable leading expert in this domain.
What to expect after an oophorectomy?
If you have gotten a bilateral oophorectomy, you may experience symptoms of menopause such as:
- Hot flashes
- Vaginal dryness
- Depression
- Decreased sex drive
Your doctor might start you on hormonal or non-hormonal medications to accustom your body to these changes and decrease the unpleasant symptoms that you might experience.
In case you have to remove both of your ovaries for medical reasons and you still wish you can have future pregnancies, discuss the option of egg freezing with your doctor.
Call us or request an appointment with Dr. Gaby Moawad to address your condition.
